
Audio By Carbonatix
A debate is raging over proposals that a second vaccine be introduced to fight Ebola in Democratic Republic of Congo, currently in the grip of its worst outbreak.
The DR Congo Health Minister, Dr Oly Ilunga, who resigned after being stripped of management of the country's Ebola response, said the current vaccine is the only one that has been proven to be effective, and an opposition MP said the new vaccine is untested, and fears people in the country will be used as guinea pigs.
Leading health experts say the second vaccine is safe and could be an important tool in holding back the spread of the virus.
So what are the concerns, and are they justified?
 Image copyrightGETTY IMAGES
Image caption A woman being screened for Ebola
Image copyrightGETTY IMAGES
Image caption A woman being screened for Ebola
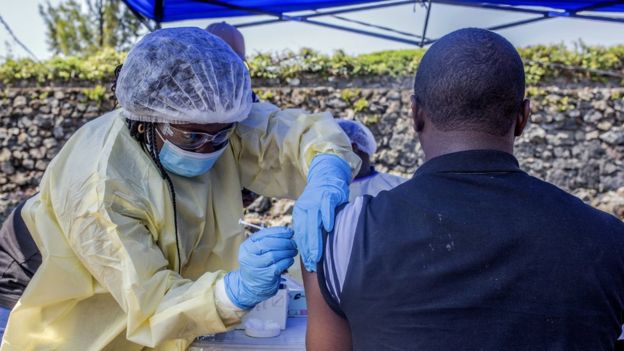 Image copyright GETTY IMAGES
Image caption A man receives a vaccine in DR Congo
Image copyright GETTY IMAGES
Image caption A man receives a vaccine in DR Congo
Tried and tested?
It has been tested on 6,000 people and "has shown outstanding safety," says Professor Peter Piot, a leading expert on Ebola and director of the London School of Hygiene & Tropical Medicine, which has been involved with pharmaceutical company Johnson & Johnson in the development of the vaccine. Studies have shown that although the drug is still in the experimental phase and hasn't been tested on patients with Ebola, it has proved highly effective in tests on primates (animals genetically close to humans). The only way to test it on humans is for it to be used in an outbreak scenario, as it wouldn't be safe to trial the medicine on volunteers infected with the virus in a clinical trial. This is how the first vaccine - by the Merck & Co drug company - was successfully deployed in Guinea in 2015. It was rolled out for "compassionate use" which allows for the use of an unlicensed drug (licenses can take years or decades to get) when no other options are available, but only with authorisation from the government of the affected country.- Ebola: One year on from Democratic Republic Congo outbreak
- The impact of militant attacks in DR Congo
- Rwanda shuts border with DR Congo to stop spread of virus
 Image copyrightGETTY IMAGES
Image caption A woman being screened for Ebola
Image copyrightGETTY IMAGES
Image caption A woman being screened for Ebola
Is there enough vaccine?
If there's already a vaccine which has been proven effective against Ebola, why not just roll out more of it? In July, the WHO Emergency Committee said it "recognises the shortage of supply" of the Merck vaccine. Dr Josie Golding of the Wellcome Trust, says it's likely there won't be enough of the vaccine to deal with the current outbreak. "If so, this would have devastating consequences. We strongly believe there is an urgent need to deploy and assess a second Ebola vaccine, developed by Johnson and Johnson." In the short term, the available doses of the vaccine may be sufficient, but not if the outbreak persists. The Merck drug firm says there is enough vaccine to immunise nearly 500,000 individuals at the current dose, and is in the process of producing more. About 1.5 million doses of the vaccine are available. There are around 10 million people in the two affected provinces combined. The current vaccine is only being given to health workers and people who might have been exposed to the virus. So, if DR Congo's government wants to roll out immunisation across a wider area, it will need more supplies. Those pushing for the use of the new Johnson & Johnson vaccine, had proposed using it to create a protective wall, vaccinating people outside the outbreak zone. It is hoped this would prevent the virus from spreading. Image copyright GETTY IMAGES
Image caption A man receives a vaccine in DR Congo
Image copyright GETTY IMAGES
Image caption A man receives a vaccine in DR Congo
Community mistrust
The DR Congo government has cited concerns about the complexities of using two vaccines together in the response. It says there is a risk of creating confusion and increasing mistrust among affected communities. The fight against the current Ebola epidemic has been marked by community mistrust towards the response. There are also concerns that the new vaccine - which requires two injections 56 days apart - may be difficult to administer in a region where the population is highly mobile, and insecurity is rife.DISCLAIMER: The Views, Comments, Opinions, Contributions and Statements made by Readers and Contributors on this platform do not necessarily represent the views or policy of Multimedia Group Limited.
Tags:
DISCLAIMER: The Views, Comments, Opinions, Contributions and Statements made by Readers and Contributors on this platform do not necessarily represent the views or policy of Multimedia Group Limited.
Latest Stories
-
World Cup 2026: Black Stars players to receive $100,000 as appearance fee – Sports Minister
2 hours -
Nigerian retired general abducted with his wife in the north-west
2 hours -
TTU crowned Overall Best Innovator at ARCTUG 2026
2 hours -
NPP members oppose resumption of Asante Mampong polling station elections
3 hours -
Educators, traditional leaders call for stronger link between humanities and skills development
3 hours -
Severe rainstorm wreaks havoc at Adaklu Kodzobi Ando
3 hours -
Hundreds arrested and dozens of police injured after Champions League riots in France
3 hours -
AMECO launches 80th anniversary with a focus on infrastructure development
3 hours -
Health Ministry receives pulse oximeter donation to support Free Primary Healthcare initiative
3 hours -
Will controlling hostel rents solve the accommodation challenges on our campuses?
3 hours -
2026 U17 WWCQ: Black Maidens to face Senegal in final round
3 hours -
McDan graces Hitz Rep Ur Jersey at Aviation Social Centre, makes commentary debut in UCL final
5 hours -
Damang Gold Mine invests $250 million in mining equipment
6 hours -
Richard Ankomah beats competition to win Hitz FM Rep Ur Jersey 2026 Quiz
7 hours -
Afriyie Wutah marks birthday with ‘Summer Jam’ featuring Maxi Priest
7 hours

