
Audio By Carbonatix
In global health, vaccines save lives, medicines cure disease, and surveillance stops outbreaks – and sanitation makes all of them work better. Far from being an “either-or” alternative to vaccines or treatments, improved sanitation is the foundation that enables immunisations and medical care to deliver their full impact.
For low- and middle-income countries (LMICs) facing infectious disease burdens, rising antimicrobial resistance, and recurring epidemics, sanitation is a low-regret, high-return investment: it consistently yields broad health benefits under almost any scenario, with minimal downside risk.
Rather than replacing modern medical tools, it complements and amplifies them – a synergy that policymakers and donors can no longer afford to ignore.
Layered Protection, Stronger Together
Modern public health relies on layers of protection. Vaccines reduce individuals’ susceptibility to infection; medications reduce the severity of illness and save lives; vector control interrupts disease transmission; and disease surveillance enables rapid outbreak response. Sanitation plays a different but equally critical role: it reduces exposure at the source, cutting off multiple pathways by which pathogens spread.
The effect is not competition but synergy. When communities are not constantly exposed to fecal pathogens in their water, food, and environments, vaccines prevent more infections. When reinfections are less frequent, antibiotics remain effective longer and need to be used less often. And when the baseline burden of preventable disease is lower, health workers and clinics can focus their resources on other pressing needs.
In short, sanitation strengthens the entire continuum from prevention to care. It creates healthier conditions in which all other interventions – from immunization campaigns to drug therapies – can perform to their fullest potential.
Reaching Diseases Vaccines Can’t
Vaccines are among the most powerful public health tools ever devised, but by design they are pathogen-specific, targeting one microbe at a time. Sanitation is not so limited. Improved sanitation and hygiene practices – such as safe disposal of human waste, clean drinking water, and handwashing – reduce transmission of a wide array of infections, including diarrheal diseases, intestinal parasites, enteric fevers, polio, and many neglected tropical diseases for which no vaccine exists.
This broad-spectrum impact fills critical gaps that biomedical tools alone cannot cover. Even where vaccine coverage is high, poor sanitation sustains the spread of pathogens beyond the reach of current vaccines or treatments. In communities with better sanitation, children are generally healthier and better nourished – factors linked to stronger immune responses and improved vaccine effectiveness.
Sanitation therefore serves as a platform for immunization. By reducing overall environmental pathogen load, it ensures that no major transmission route is left unaddressed, allowing vaccines to confer maximum protection.
A Quiet Ally Against Antimicrobial Resistance
Every avoidable infection prevented through sanitation is an infection that does not require antibiotics, helping slow the rise of antimicrobial resistance (AMR) in LMICs. Where sanitation systems are weak, resistant bacteria and resistance genes spread easily through water, soil, and human contact. This drives a vicious cycle of infection and antibiotic use.
Improved sanitation breaks this chain. By safely removing fecal contamination from communities, it reduces infections requiring treatment, lowers antibiotic consumption, and limits environmental dissemination of resistant organisms. In this way, sanitation acts as a powerful non-pharmaceutical AMR intervention, working alongside stewardship programs and drug development.
Ending open defecation and improving basic waste management has already shown dramatic reductions in diarrheal disease mortality in some settings. Scaled globally, similar improvements could significantly reduce resistant infections, particularly when paired with more prudent antibiotic use. Sanitation helps preserve existing medicines by reducing the demand placed on them.
Resilience to the Next Outbreak
The COVID-19 pandemic demonstrated that basic sanitation and hygiene are pillars of outbreak resilience. Before vaccines or treatments were available, societies relied on fundamentals such as hand hygiene, clean water, and safe sanitation to curb transmission – especially in resource-limited settings.
Strong sanitation systems mean fewer opportunities for diseases like cholera, typhoid, or novel pathogens to spread rapidly. Health facilities are safer, baseline disease burden is lower, and communities are better positioned to comply with public health guidance.
Sanitation therefore builds an all-hazards shield: it reduces everyday infectious disease while providing durable infrastructure that underpins emergency response. Every pandemic preparedness plan should include accelerated access to safe water and sanitation – investments that deliver daily benefits while strengthening resilience against future threats.
“Low-Regret” Means High Reward
Sanitation is the quintessential low-regret investment. Even conservative estimates show that basic sanitation yields large health gains at relatively low cost, with the biggest returns coming from the earliest, simplest improvements.
Providing improved latrines and hygiene education can reduce diarrheal disease substantially, lower parasite infections, improve nutrition, and increase school attendance. Economic returns are strong, driven by reduced health-care costs and increased productivity.
Critically, large benefits do not require expensive sewer systems at the outset. Simply ending open defecation and ensuring safe containment of waste produces outsized gains that pay for themselves many times over. By contrast, the cost of inaction is immense: preventable illness, child mortality, lost education, reduced economic potential, and recurring public health emergencies.
Few interventions so reliably complement other priorities – from education and gender equity to economic development and climate resilience – as sanitation.
Comparing Preventive Interventions
All core public health tools are essential, but sanitation stands out as the platform that underlies and enhances the rest.
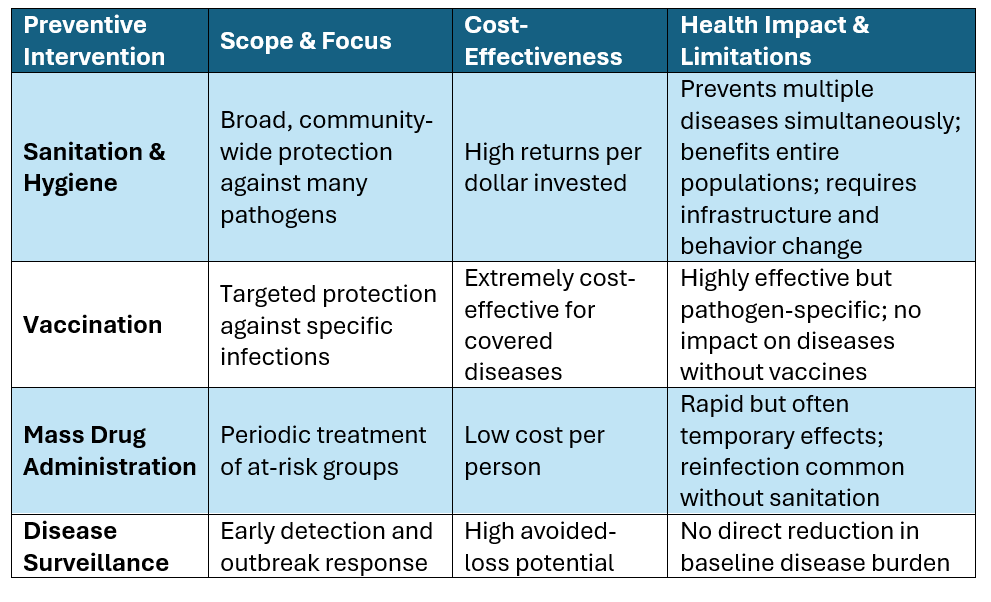
For maximal health security, basic sanitation, immunization, appropriate medication, and surveillance must work in tandem.
Integration as Core Policy, Not an Afterthought
The evidence is overwhelming: sanitation is central to achieving health goals, from reducing child mortality and malnutrition to controlling neglected diseases and strengthening health security. Yet it is still too often treated as separate from health policy.
This must change. Vaccines, treatments, surveillance, and sanitation are all strongest when deployed together. Health ministries should coordinate with water and sanitation agencies to target disease hotspots. Donors supporting immunization or AMR efforts should invest in complementary sanitation improvements to protect the returns on their investments.
Every health clinic should have safe water and toilets. Every vaccination campaign in underserved areas is an opportunity to advocate for sanitation. Financially and ethically, integration makes sense.
Conclusion
Vaccines save lives. Treatment cures disease. Sanitation makes both sustainable.
Health gains achieved through medicine and immunization will be difficult to maintain if billions of people still lack safe sanitation. By undergirding all other interventions, sanitation is the bedrock of healthier, more productive societies.
The false choice between sanitation and medicine must be abandoned. Rather than competing with vaccines or clinics, sanitation underpins their success. Prioritizing sanitation now is a high-impact, low-regret strategy that will save lives, strengthen health systems, and ensure the benefits of modern medicine reach everyone.
Latest Stories
-
IMF says BoG’s multi-billion cedi losses were part of economic recovery
37 minutes -
The losses were necessary – IMF backs BoG’s costly economic rescue
1 hour -
People on the ground recognise the gains – IMF backs BoG strategy
1 hour -
Oil prices slide on hopes of US-Iran peace deal
2 hours -
Italy busts €300 million streaming piracy ring
2 hours -
Texas sues Meta, WhatsApp over encryption privacy claims
2 hours -
US appeals court revives $82 million of verdict against Ford in trade secrets case
2 hours -
Activision shareholders reach $250m settlement over Microsoft buyout
2 hours -
Google appeals US court ruling on search monopoly
2 hours -
QNET, Manchester City Host Grassroots Football Clinic in Ghana
3 hours -
StanChart CEO Bill Winters apologises for ‘upset caused’ by AI comments
3 hours -
Grok falls flat in Washington, undercutting SpaceX’s AI growth story
3 hours -
Bank of Ghana was not too aggressive – IMF defends tight policy measures
3 hours -
Stakeholders demand urgent intervention in Ghana Swimming Association crisis
5 hours -
Labourer remanded for allegedly robbing financial consultant
5 hours

