Audio By Carbonatix
One person in the Upper East Region has been confirmed dead after testing positive for monkeypox.
The Upper East Regional Director of Health Services, Dr Emmanuel Kofi Dzotsi confirmed this to JoyNews. According to him, this is the region’s first monkeypox case.
In a press release, he indicated that "the confirmed case was seen on the 22 July 2022 at the Upper East Regional Hospital with history of fever and skin rash."
"Unfortunately, the case died on the 26th of July 2022. Samples were taken on July 22, 2022, for confirmation at the Noguchi Memorial Institute for Medical Research (NMIMR) in Accra. We received feedback on July 28, 2022, indicating the sample tested positive for Monkeypox disease."
Dr Dzotsi added that 13 contacts close to the confirmed case have been identified for contact follow-up and monitoring.
"As of 31st July 2023 no additional cases have been confirmed," he stated.
Meanwhile, the monkeypox outbreak has been declared a global health emergency by the World Health Organization.
The classification is the highest alert that the WHO can issue and follows a worldwide upsurge in cases.
More than 16,000 cases have now been reported from 75 countries, said WHO director-general Dr Tedros Adhanom Ghebreyesus.
There are only two other health emergencies currently – the coronavirus pandemic and the continuing effort to eradicate polio.
About monkeypox
Monkeypox is endemic in countries such as Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Ghana, Ivory Coast, Liberia, Nigeria, the Republic of the Congo, Sierra Leone, and South Sudan.
Transmission of virus
Transmission occurs primarily via respiratory droplet particles usually requiring prolonged face-to-face contact, which puts household members of active cases at greater risk of infection.
Transmission can also occur via inoculation or the placenta (congenital monkeypox). There is no evidence, to date, that person-to-person transmission alone can sustain monkeypox infections in the human population.
Secondary, or human-to-human, transmission can result from close contact with infected respiratory tract secretions, skin lesions (open wounds/injuries) of an infected person or objects recently contaminated by patient fluids or lesion materials.
Symptoms
The infection can be divided into two periods:
The invasion period (0-5 days) characterised by fever, intense headache, lymphadenopathy (swelling of the lymph node), back pain, myalgia (muscle ache) and an intense asthenia (lack of energy);
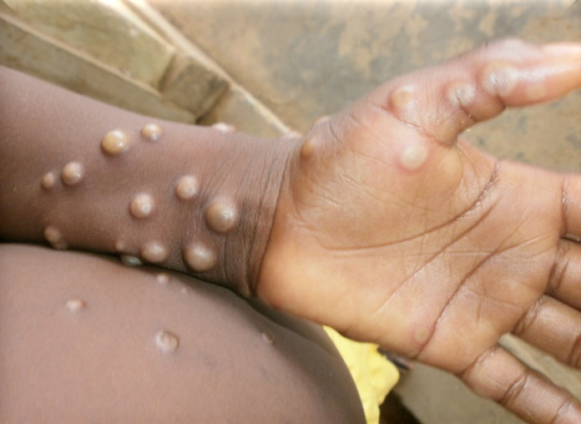
The skin eruption period (within 1-3 days after the appearance of fever) where the various stages of the rash appears, often beginning on the face and then spreading elsewhere on the body.
The face (in 95% of cases), and palms of the hands and soles of the feet (75%) are most affected.
Treatment/Vaccine
There are no specific treatments or vaccines available for monkeypox infection, but outbreaks can be controlled.
Vaccination against smallpox has been proven to be 85% effective in preventing monkeypox in the past but the vaccine is no longer available to the general public after it was discontinued following global smallpox eradication.
Prevention
In the absence of specific treatment or vaccine, the only way to reduce infection in people is by raising awareness of the risk factors and educating people about the measures they can take to reduce exposure to the virus.
Regular hand washing should be carried out after caring for or visiting sick people.
Reducing the risk of animal-to-human transmission. Efforts to prevent transmission in endemic regions should focus on thoroughly cooking all animal products (blood, meat) before eating.
Public health educational messages via the media – broadcast, electronic and social – is highly advised.
Healthcare workers and those treating or exposed to patients with monkeypox or their samples should consider being immunized against smallpox via their national health authorities.
Latest Stories
-
Cobolli using Nadal’s shower in bid for French Open glory
4 hours -
Director Wim Wenders withdraws 1975 film over actress’s teen topless scene
4 hours -
Berrettini tired of retiring as injury strikes again
4 hours -
Sabalenka lets another golden Slam opportunity slip
5 hours -
Man shot dead by FBI after taking hostages at California bank
5 hours -
‘Crazy’ phone call between Trump and Netanyahu complicates Iran talks
5 hours -
Shell pumped oil through Nigeria pipeline for years despite pollution evidence, documents show
5 hours -
Meta workers can opt out of being tracked at work – but only for half an hour at a time
5 hours -
DACF, Wahu Mobility partner to roll out 5,000 electric motorcycles across Ghana
5 hours -
US announces new tariffs over forced labour concerns
5 hours -
One dead, 2 remain trapped after building collapse at Adenta
6 hours -
‘You’ve Done Very Well’: Multimedia COO Ken Ansah applauds Jeffrey Nortey’s journey and pledges support
6 hours -
Fire destroys parts of Makola Market
6 hours -
Multiple people trapped after storey building collapsed at Adenta New Site
6 hours -
Parts of Accra flood again after Wednesday downpour
7 hours